Types of children's brain tumours
Medulloblastoma develops at the back of the brain in the cerebellum.

Around 52 children are diagnosed with medulloblastoma each year in the UK. Adults can also get this type of tumour, but it is rare.
Medulloblastoma is likely to grow quickly and can spread to other areas of the brain and spinal cord. Around 30 out of 100 children (around 30%) have medulloblastoma that has spread when they are first diagnosed.
Recently, research has been able to identify new types and subtypes of medulloblastoma. This is due to the discovery of specific genetic and molecular information.
Doctors used to talk about medulloblastoma as a primitive neuro ectodermal tumour (PNET). This term is no longer used.
Medulloblastoma can affect children of any age, but it is most common in children aged 5 to 9. It is more common in boys than girls.
Most people worry about what caused their child to develop cancer. We don’t know what causes most childhood cancers or how to prevent them. This includes medulloblastoma.
We know there is an increased risk of medulloblastoma with some inherited family cancer syndromes. But remember, not every child with one of these syndromes develops medulloblastoma. Less than 5 out of every 100 cases of medulloblastoma (less than 5%) are linked with either:
familial adenomatous polyposis (FAP) - sometimes known as Turcot syndrome
nevoid basal cell carcinoma syndrome (NBCCS) – also known as Gorlin syndrome
Find out about possible causes and risks of cancer in children
Your child might have symptoms for a few weeks or months before they are diagnosed with medulloblastoma. Many symptoms are general and non specific. Some are similar to less serious childhood illnesses. Symptoms might include:
headaches in the morning
feeling or being sick – being sick often makes the headaches feel better
double vision
finding it hard to sit or stand unsupported – your child might often fall backwards
being more fractious or irritable – it might be taking longer than usual to get your young child to settle
loss of appetite
behaviour changes – they might be interacting with you or their siblings less
During a young infant’s routine development check up, symptoms sometimes picked up are:
an increasing head size (head circumference)
a swollen soft spot on top of the skull (fontanelle)
Take your child to your GP if you are worried your child has a symptom of a brain tumour.
Find out more about symptoms of brain tumours in babies, children and teenagers
The first tests your child might have are:
a CT scan
an MRI scan
They might also have a . This is a test to check for cancer cells in the fluid that surrounds the brain and the spine. This fluid is called cerebrospinal fluid (CSF). Your child’s doctor or specialist nurse will take a sample from the fluid around their spine.
For some types of test, your child might need or a . This is to help them lie still.
We have information about tests for children’s brain tumours and how to prepare
Researchers are learning more about medulloblastoma all the time. At the moment, it’s grouped by what the cells look like under the microscope. Your child’s doctor needs a sample of the tumour to work out which type it is. This means they won’t be able to tell you straight away about what type it is.
There are 4 types:
classical medulloblastoma – around 8 out of 10 children (around 80%) have classical medulloblastoma
anaplastic or large cell medulloblastoma
nodular or desmoplastic medulloblastoma – this type is most common in infants
medulloblastoma with extensive nodularity (MBEN)
Using new techniques, scientists can also look inside the medulloblastoma cells at the genes and proteins. This means we can now group medulloblastoma into 4 further subtypes. These are:
subtype 1 – wingless (WNT) medulloblastoma
subtype 2 – sonic hedgehog (SHH) medulloblastoma
subtype 2 – group 3 medulloblastoma
subtype 4 – group 4 medulloblastoma
Knowing about the different subtypes of medulloblastoma helps doctors understand the tumour better. This includes how well treatment might work.
Researchers want to learn more about these differences in medulloblastoma. They hope to make treatments targeted to these subtypes in the future.
The main treatments for medulloblastoma are:
surgery
radiotherapy
chemotherapy
Each child has their own treatment plan. Surgery is usually the first treatment your child will have. Rarely some children have chemotherapy first to shrink the tumour before surgery.
Your child’s specialist team decides on the best treatment for your child. Both you and your child will be involved in decisions about treatment and care.
Surgery is usually the first treatment your child will have.
Your child has surgery to remove as much of the tumour as possible. At the same time, your child’s surgeon takes a piece of the tumour to look at under the microscope. This is to find out what type of medulloblastoma it is.
Hearing your child needs brain surgery can feel very frightening. A paediatric neurosurgeon does the operation. They’re highly skilled professionals in looking after children with brain tumours.
Some tumours cause a fluid build up in the brain. This is called hydrocephalus. This can cause symptoms. Some of the symptoms might include:
headaches
feeling or being sick
seizures (fits)
problems with their eyes or vision
problems with their strength, balance or coordination
changes in their behaviour
Treatment to reduce this is an operation. Your child’s surgeon can do this at the same time as removing their tumour.
They might either:
make a hole to drain fluid into another area of the brain (ventriculostomy)
put a tube in their head so that the fluid drains from the brain to another part of the body (a shunt). This is usually into the tummy (abdomen) where the body gets rid of it
Posterior fossa syndrome is a group of symptoms that happens after surgery to the back of the brain. Around 25 to 30 out of 100 children (around 25 to 30%) get posterior fossa syndrome. Symptoms can include:
difficulty talking, such as not speaking or their speech might be slurred or slow
difficulty swallowing
trouble with their muscle tone and being able to move. Symptoms might include your child finding it difficult to walk, or unable to sit up
being unable to control their movements, so they may make sudden movements. This can look like they are twitching or jerking, or you might notice their eyes moving from side to side
poor balance
weakness on one side of the body
changes in their mood and behaviour, which doesn’t fit the situation or is out of character for them
The symptoms can be very mild or severe. There is no way to know how or if your child will be affected. The symptoms usually develop from one day to a week after surgery.
Posterior fossa symptoms usually improve slowly over a few weeks or months. But they may not go away completely in some children. Research is trying to find out what causes posterior fossa syndrome.
After surgery, your child has some more tests, usually an MRI scan and lumbar puncture. This is to work out if there is any cancer:
left after the operation and if so, how much there is
in the fluid that surrounds the brain and spinal cord (CSF)
The doctor decides on further treatment based on the results of the tests and other factors. These include:
what the cells look like under the microscope – the type of medulloblastoma
if the medulloblastoma has spread
how old your child is
Based on these factors, your child goes into one of two treatment groups. These are based on the risk of medulloblastoma coming back after treatment. These groups are:
high risk
standard risk
Your child only needs one of these factors to be in the high risk group:
they are under 3 years old
they have medulloblastoma that has spread
their surgeon was not able to remove all the tumour, and the tumour that is left is more than 1.5cm2 in size
they have large cell or anaplastic medulloblastoma
they have certain gene changes
Every child in the standard risk group is:
3 years or over
their surgeon removed all of their tumour, or they only have a very small amount left
their medulloblastoma has not spread and doesn’t have any features that make it high risk
All children under the age of 3 are in the high risk group.
Your child’s specialist usually avoids using radiotherapy to the whole brain and spine if your child is younger than 3. This is to reduce the risk of developing long term side effects, which is higher in children younger than 3.
Chemotherapy is the use of anti cancer drugs to destroy cancer cells.
Your child’s specialist might recommend chemotherapy instead of whole brain and spine radiotherapy. This aims to keep your child's tumour under control until radiotherapy is likely to cause less damage.
Medulloblastomas in young children are more often desmoplastic tumours. These tumours are sensitive to treatment and can often be successfully treated with chemotherapy on its own. Your child has chemotherapy using several different drugs. They have these into their bloodstream, through a drip (intravenous chemotherapy).
Chemotherapy drugs your child might have include:
cisplatin
cyclophosphamide
vincristine
etoposide
methotrexate
carboplatin
Get more information on cancer drugs including side effects
Children with desmoplastic tumours might also have chemotherapy (methotrexate) into the cerebrospinal fluid (CSF). During surgery, the surgeon might put a plastic dome under the skin of your child’s scalp. It's called a ventricular access device or an Ommaya reservoir. They inject the chemotherapy through the Ommaya reservoir. This is called intraventricular chemotherapy.
Some children with other types of medulloblastoma might have high dose chemotherapy then an .
The exact treatment plan depends on your child’s risk group if they are over 3 years old.
Generally, children over 3 years old have:
chemotherapy
radiotherapy to the brain and spine
Some children aged between 3 and 6 years have chemotherapy only without radiotherapy. The doctor will go over the risks and benefits of this treatment with you, if this is an option for your child.
Your child might have a combination of chemotherapy drugs during or after radiotherapy.
The chemotherapy drugs your child might have include:
cisplatin
lomustine
vincristine
cyclophosphamide
carboplatin
topotecan
Find out more about having chemotherapy for a childhood brain tumour
Radiotherapy means the use of radiation, usually x-rays, to treat cancer. Radiotherapy is a treatment used to try to cure cancer, reduce the chance of cancer returning, or to help with symptoms.
There are different ways to give radiotherapy. For medulloblastoma, children receive radiotherapy from outside the body (external radiotherapy).
Radiotherapy machines are very big. They usually rotate around your child to give treatment. But they don’t touch your child at any point.

Your child needs to keep still for their radiotherapy. For some young children, this means they need a general anaesthetic to help them lie still. Each individual dose, or fraction, of radiotherapy is quick and painless.
Children’s radiotherapy teams are used to treating children with brain tumours. A play specialist will help your child prepare and cope with radiotherapy.
It can be daunting for you, so the team will make sure you know what to expect. Ask them any questions you have.
Radiotherapy usually starts around 4 to 6 weeks after surgery. Your child might have radiotherapy for 6 weeks.
Find more information on radiotherapy for children’s brain tumours
Proton beam therapy is a type of radiotherapy. It uses protons rather than high-energy x-rays to kill cancer cells. Protons are tiny parts of atoms. They work differently from x-rays. They produce a sudden burst of energy when they stop, which stays inside the tumour. So, there is less damage to healthy cells around the tumour.
Children with standard risk medulloblastoma usually have this treatment.
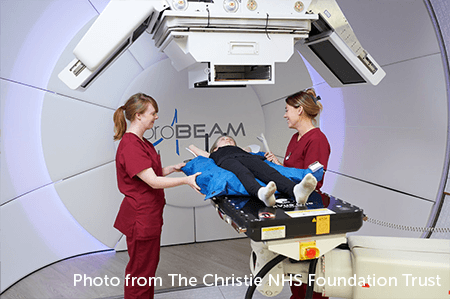
Your child’s specialist will talk with you if they think proton therapy might be helpful for your child.
There are 2 proton beam therapy centres in the UK. These are at:
The Christie Hospital in Manchester
University College London Hospital
University College London Hospital opened in 2021. They’re gradually opening their service to the rest of the UK.
At the moment, children who need this treatment will have to travel to one of these hospitals or abroad for it.
Find out more about proton beam therapy
Some children with high risk medulloblastoma might have high amounts (doses) of chemotherapy, followed by a stem cell transplant. This kind of transplant is called an autologous transplant, autograft or auto transplant.
An autologous transplant uses your child’s own to replace blood cells destroyed by high doses of chemotherapy. Some children might also have radiotherapy.
A nurse collects your child’s stem cells from their bloodstream through a drip. If they have this type of collection they will have injections first. The growth factor causes the stem cells to spill into the blood from the bone marrow. When they have enough stem cells, they collect them through a drip from their bloodstream.
Rarely, your child might have stem cells collected from their . They have this under general anaesthetic. The doctor puts a needle into your child’s hip bone to remove the stem cells.
Before an autologous transplant, your child has treatment to prepare their body to receive the stem cells. You might hear this called conditioning treatment. The conditioning treatment kills cancer cells, as well as healthy cells in your child’s blood, bone marrow and other parts of the body. This also helps make space in their bone marrow to receive the stem cells.
It’s harder to treat medulloblastoma that has not gone away with treatment (refractory) or has come back (relapsed).
Treatments for children with refractory or relapsed medulloblastoma might include:
surgery
radiotherapy
chemotherapy – usually tablets or liquids taken by mouth
a targeted cancer drug
joining a clinical trial
Your child’s specialist will talk with you about the possible treatments for your child. They will involve you in any decisions about their treatment and care. Ask them any questions you have.
The side effects of treatment are different for each child. Some side effects of chemotherapy and radiotherapy happen during treatment and stop once treatment finishes. Other side effects happen months or years after treatment. These are late side effects or long term effects. They can be mild or more challenging. Not all children have challenging long term side effects.
To help them with any long term side effects, a team of specialists will closely check your child after treatment finishes.
The possible side effects of treatment could lead to problems at school or with your child meeting their developmental milestones.
We have information on follow up and late effects of children’s brain tumour treatment, what treatments can help, and where to get support. The brain tumour late effects service will provide long term support for your child.
Find out about follow up and late effects
Researchers are interested in finding new and kinder ways to treat medulloblastoma. And ways to reduce the side effects of treatment. Many children have their treatment for a brain tumour as part of a clinical trial.
Read more about clinical trials looking into children’s brain tumours here
We have information about where to get help and support to help you and your child cope.
Find out about coping with cancer
This page is due for review. We will update this as soon as possible.
Last reviewed: 03 Jan 2023
Next review due: 03 Jan 2026
Tumours affecting the brain and central nervous system are the second most common type of children’s cancer in the UK. Around 420 children are diagnosed with these tumours each year in the UK.
Brain tumour symptoms can be very similar to those of childhood illnesses. Take your child to the GP if they have any symptoms of a brain tumour.
The main treatments for children’s brain and spinal cord tumours are surgery, radiotherapy and chemotherapy.
We don't know what causes or how to prevent most childhood cancers. There are some factors that can increase the risk of cancer in children.
It is essential that parents and other close family have support. Find out what is availble and who can help.
There are over 100 different types of tumour that can develop in the brain or central nervous system. They are usually named after the type of cell they develop from. Find out more about the different types.

About Cancer generously supported by Dangoor Education since 2010. Learn more about Dangoor Education
Search our clinical trials database for all cancer trials and studies recruiting in the UK.
Connect with other people affected by cancer and share your experiences.
Questions about cancer? Call freephone 0808 800 40 40 from 9 to 5 - Monday to Friday. Alternatively, you can email us.